What is calciphylaxis?
Calciphylaxis (also known as calcific uraemic arteriolopathy) is a rare condition that can develop in people receiving dialysis for kidney failure. It occurs when calcium and phosphate build up in the body, causing chalky deposits in the small blood vessels (calcification).
This leads to a narrowing of the blood vessels, which reduces the blood supply to parts of the body such as the heart, soft tissues and skin. This can cause skin ulcers that take a long time to heal and may become infected, as well as damage to the body’s organs.
Calciphylaxis affects around 1 in 10,000 people in the UK and occurs in 1 in 600 people receiving dialysis. It is usually diagnosed in late adulthood and is more common in women than men – although the reason for this is unknown.
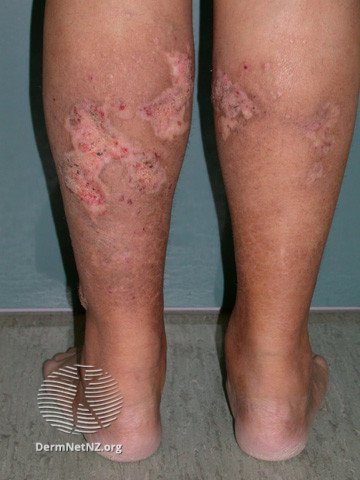
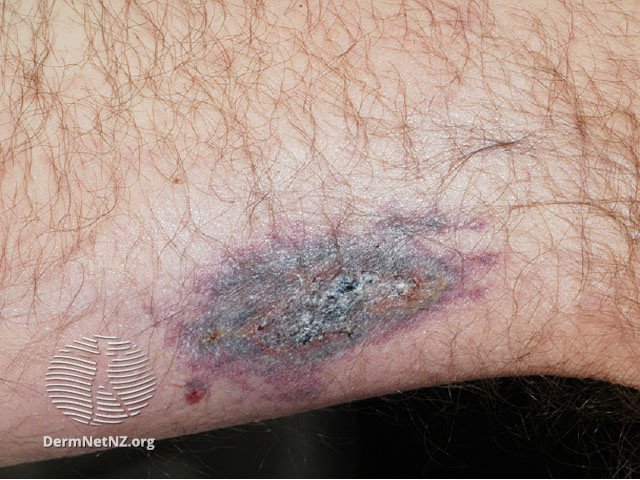
Calciphylaxis skin ulcers images © DermNetNZ
What are the signs and symptoms of calciphylaxis?
Calciphylaxis can make people feel very tired and unwell, although this may be more of a symptom of dialysis rather than the condition itself.
Calciphylaxis causes ulcers to develop on the skin. These usually occur on the legs and abdomen but can affect any part of the body. The ulcers can be extremely painful and can become infected.
What causes calciphylaxis?
The exact cause of calciphylaxis is currently unknown. It is sometimes triggered by a small injury such as an insect bite or a cut. Other risk factors that appear to make people more likely to develop calciphylaxis include:
- being overweight
- having high levels of calcium and/or phosphate in the blood
- being on dialysis for a long period of time
- having diabetes
- taking warfarin (a medication to thin the blood).
How is calciphylaxis diagnosed?
Calciphylaxis is usually diagnosed by a clinical examination. A skin biopsy may be used to look for calcification, but this is risky as it can cause a wound that also doesn’t heal because of the calciphylaxis. Biopsies may therefore only be used for unusual-looking ulcers or skin lesions.
Does calciphylaxis affect other parts of the body?
Although calciphylaxis occurs as a result of kidney damage, it mostly affects the skin, causing extremely painful ulcers that can become infected.
It can also affect the heart, as calcium deposits can block the blood vessels, increasing the risk of having a heart attack and leading to the need for heart valve replacements.
Does calciphylaxis run in families?
Calciphylaxis is not a genetic condition, so it does not run in families.
How is calciphylaxis treated?
There is currently no specific treatment for calciphylaxis, although several clinical trials are researching possible options. Clinical management focuses on:
Supportive care
- pain management
- wound care – keeping any cuts clean to try and prevent infection
- skin creams
- good nutrition to promote healing
Managing risk factors
- dietary changes to limit high-phosphate foods such as cheese and nuts
- altering the dialysis schedule by moving to more frequent and/or longer sessions
- changing from peritoneal dialysis to haemodialysis to control the mineral losses
- changing the dialysate (the fluid used for dialysis) to one with lower calcium
- varying the sites of any daily injections, like insulin, to prevent infection
Managing medications
- stopping medication that may make calciphylaxis more likely to occur. This may include warfarin, active vitamin D, calcium-based phosphate binders, calcium supplements and thiazides (a blood pressure medication)
- prescribing new medication to lower the levels of calcium and/or potassium in the blood, as well as blood pressure medication to protect the heart
If the ulcers become infected, hospital treatment may be needed. In very severe cases the affected limb may need to be amputated, but this can make the situation worse as the new wound is unable to heal properly.
Half of all people with calciphylaxis die within a year of diagnosis. Death usually occurs because of infection from the ulcers.
Where can I get more information or support about calciphylaxis?
For more information on calciphylaxis including its diagnosis, symptoms and treatment, visit the UK Calciphylaxis Study

Publication date: 11/2023
Review date: 11/2026